Which Type Of Collagen To Take? (Joints,Hair, Skin, Nails, Muscle)
Collagen is a protein that can help with joint pain and soft tissue recovery. However, many supplements exist on the market, and you may have noticed different types of collagen, for example, collagen I, II, II, IV and so on.
Even though the different types of collagen have distinct and essential roles in the body, you do not have to take separate supplements to build up these collagens as they are all composed of the same amino acids: glycine, proline, and hydroxyproline. As long as you get enough of these amino acids at the right time (60 – 90 min before a workout) with a source of vitamin C, your body can build the different types of collagen you need.
However, it is good to understand what the different types of collagen do in the body, why you need to take in enough collagen, and how to interpret different supplement labels.
What Is Collagen?
Collagen is a vital part of the structure of tissues that gives them flexibility. In muscles, connective tissue helps transmit the force of muscle contractions to tendons and bones.
The proteins in connective tissue are constantly changing, and they can adapt. Eating protein boosts the synthesis of muscle proteins.
Proteins that are high-quality and easy to digest are usually recommended for best results. Interestingly, recent studies show that protein intake doesn’t increase the production of proteins in muscle connective tissue.
This lack of increase might be due to insufficient glycine and/or proline. Collagen-rich foods containing plenty of glycine and proline are suggested to provide the building blocks for connective tissue protein synthesis [1].
In the body, collagen is like the scaffolding that holds everything together. Imagine it as the essential building block that maintains the health of our skin and connective tissues [2].
“Connective tissue” is the supportive framework that binds our organs and tissues. It comprises fibroblasts and their extracellular matrix, a kind of scaffolding around the cells.
This extracellular matrix is vital because it ensures cells stick together, maintains stability, and aids in the regeneration process across different tissues [3].
These tissues need collagen to stay strong, flexible, and capable of repairing themselves. Collagen is part of the extracellular matrix, which is like a support network for our cells [4].
This matrix provides structure and helps regulate and renew our tissues.
Think of tendons, the tough bands that connect muscles to bones. They rely heavily on collagen, which makes up a significant portion of their weight.
Collagen’s unique structure, formed by specific amino acids like glycine and proline, gives it strength. This is particularly important for tendons to withstand the stresses and forces, like those encountered during sports activities, helping to keep them healthy and reducing the risk of injuries [5].
So, collagen is not just a protein; it’s a crucial element that keeps our body’s structural integrity in check.
Collagen forms a “triple helix,” which helps it be strong and flexible. The triple helix consists of three polypeptide chains, or protein strands, intertwined like a rope.
These chains are rich in amino acids, with glycine being the most abundant. Proline and hydroxyproline are also crucial for stabilizing the structure [2, 6].
This combination of strength and flexibility makes collagen well-suited for providing structural support in tissues like skin, tendons, and bones.
Should You Take A Specific Collagen Type?
Type I collagen is predominant within bone, muscle, and connective tissue. There is not enough research yet to say that consuming type I collagen is superior to consuming other collagen types, like type II or III, because they all contain similar building blocks – i.e., amino acids.
Interestingly, many studies also use gelatin as a collagen source when studying the impact of collagen on the body.
Once again emphasizing that the main priority is to get in the different amino acids that can build the various collagen types.
However, because type I collagen plays such a significant role in the bone, muscle, and connective tissues, it does make sense to opt for it when choosing a collagen supplement.
Different Types Of Collagen
A total of 29 exist, each designated by Roman numerals I-XXIX in order of their discovery [7, 8]. Each collagen type has unique characteristics, functions, and locations within the body [2].
Different collagen types have structural differences that help them have different bodily functions at different locations.
Its amino acid composition and arrangement determine the physical structure of collagen and how individual collagen molecules interact to form larger structures [2, 5, 9].
Here’s how the physical structure is related to the diversity of collagen types:
- Amino Acid Composition:
The amino acid composition of collagen varies among different types. For example, collagen types I and II have a high glycine, proline, and hydroxyproline content, while other types may have different amino acid compositions. This variation influences the collagen structure’s strength, flexibility, and stability [9].
- Triple Helix Structure:
The “triple helix” refers to how collagen is put together. Each structure consists of three polypeptide chains twisted around each other, almost like a rope.
Each of these chains is known as an alpha chain (remember this because we refer to it later in this post). The specific type of collagen is determined by the arrangement of these alpha chains and the characteristics of the resulting collagen structure.
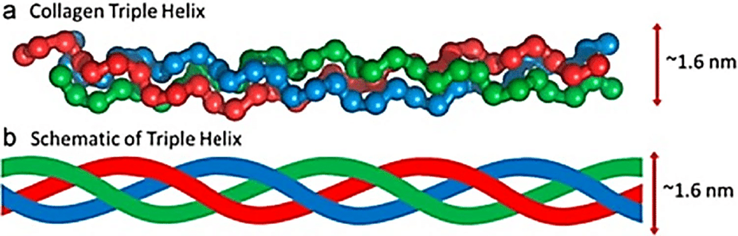
Figure 1: The collagen triple helix structure [10]
- Fibril Formation:
Collagen molecules assemble into larger structures such as fibrils and fibers [2, 9].
“Fibrils” refer to tiny, thread-like structures smaller than fibers but larger than individual molecules. Imagine them as miniature threads or strands that form a larger structure. In the context of collagen, fibrils are the building blocks of collagen fibers.
Picture a rope made of many small threads twisted together. Each of these threads can be compared to a fibril.
These fibrils join forces to create a more significant and stronger structure, similar to how the threads in a rope combine to form a robust and durable cord.
The way these structures form and the interactions between collagen molecules influence the physical properties of tissues.
- Crosslinking:
Collagen fibers are stabilized by crosslinking, chemical bonds between adjacent collagen molecules. The pattern and extent of crosslinking contribute to the strength and resilience of collagen-rich tissues, as seen in Figure 2.
Different collagen types may exhibit variations in crosslinking patterns, affecting the physical characteristics of tissues [11].
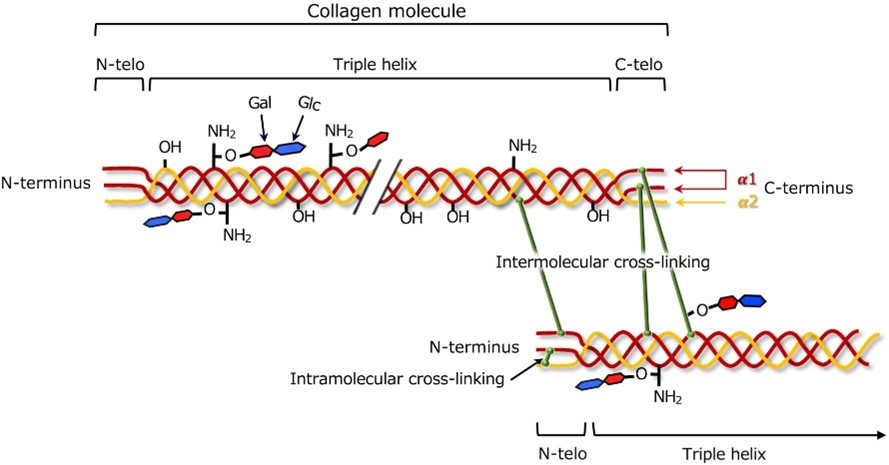
Figure 2: Collagen cross-linking [12]
Based on how they’re set up in tissues, collagens are genetically different and sorted into subgroups [13].
Collagens like I, II, III, V, and X team up to create big fibrils outside cells, earning them the name fibril-forming collagens.
Type IV collagen, on the other hand, forms a crisscrossing network in basement membranes. Then there’s type VI collagen, making unique microfibrils, and type VII collagen, creating anchoring fibrils.
A group called FACIT collagens [14] (fibril-associated collagens with interrupted triple helices), including types IX, XII, XIV, XIX, XX, and XXI, team up with the bigger collagen fibers, acting like molecular bridges.
Their job is to keep the extracellular matrix organized and stable. It’s like they’re the support crew ensuring everything stays in place.
Type I

Type I collagen is a crucial building block found in our bones, skin, and connective tissues [15]. It’s not only the most abundant type of collagen but also plays a vital role in maintaining the structure and strength of these tissues.
Think of it as the main architect, forming the basic framework for various parts of our body. Scientists have extensively studied Type I collagen because of its importance, making it the most investigated collagen type.
It is a fundamental component in almost every connective tissue, forming the primary structure of the interstitial membrane that supports and holds our body together.
Beyond its structural significance, Type I collagen finds applications in diverse medical scenarios, including surgical procedures, wound healing, and tissue engineering [16], showcasing its versatility and importance in promoting health and recovery.
Type II
Let me break it down for you: Collagen type II is the main ingredient in the structure of cartilage, which is the material that cushions and supports your joints.
About 90% of the collagen in cartilage is type II collagen [17].
The unique characteristics of Type II collagen make it essential for the resilience and shock-absorbing properties of cartilage, which is crucial for joint health.
Type 2 collagen creates a network of tiny fibers required for the cartilage’s strength [18, 19].
Collagen type II also has an important job in the growth and changes of cells (called chondrocytes) in normal cartilage development and when someone has osteoarthritis (OA), a condition that affects the joints.
When collagen type II is lost, it can speed up the growth of chondrocytes and the progression of osteoarthritis.
It happens through something called the BMP-SMAD1 pathway, which is like a communication system within the cells.
So, in a nutshell, having enough collagen type II is essential for keeping your cartilage healthy and preventing osteoarthritis from getting worse [20].
A study done in 2016 showed that using both native type II collagen and acetaminophen (a type of medication used to treat osteoarthritis) together works better for relieving symptoms in people with knee osteoarthritis than using only acetaminophen.
So, combining these two treatments seems to be more effective in helping patients manage their knee osteoarthritis symptoms [21].
Type III

Discovered in 1971, type III collagen is a major player in the collagen family, constituting about 520% of the total collagen content in our bodies. It’s like a fundamental building block contributing to structural integrity [22].
Type III collagen is also called a collagen alpha-1(III) chain, or alpha 1 chain of type III collagen [23] (remember that we mentioned that the alpha chains are the individual ropes that make up the collagen triple helix structure).
Type III collagen is a protein encoded by the COL3A1 gene in humans (this means that the gene instructs the body to make type III collagen) [23].
It is found in significant amounts in large blood vessels, the uterus, and the bowel and serves as a structural component, essentially providing a scaffold for these hollow organs.
But its importance goes beyond structure. It engages with platelets in our blood, aiding in the clotting process, and also acts as a signaling molecule during wound healing.
The significance of type III collagen becomes even clearer when studying individuals with mutations in the COL3A1 gene.
These mutations can lead to serious issues such as spontaneous ruptures in arteries, the uterus, and the bowel (your gut).
This highlights the indispensable role of type III collagen in keeping these organs structurally intact [24, 25, 26].
Interestingly, mutations in the COL3A1 gene can also result in severe brain anomalies. This suggests that type III collagen isn’t just about physical structure.
It’s also paramount for normal brain development[27, 28, 29].
So, beyond being a structural powerhouse, type III collagen plays vital roles throughout our body, influencing both physical structure and functional processes.
Type IV
Type IV collagen is a protein that’s distributed across multiple tissues, especially in an area called the basement membrane.
It can be found in various places in the body, like hair, cell surfaces, and the placenta [30].
What makes Type IV collagen interesting is its structure. At the end of its chain (C-terminus), there’s something called the C4 domain, and unlike other collagens, it doesn’t get removed during the protein-making process.
This unique feature causes the collagen fibers to link head-to-head instead of side-by-side [30].
Type IV collagen doesn’t have a specific amino acid (glycine) in every third position of its chain, which is typical in other collagen types.
This absence makes Type IV collagen more flexible and curved in its overall shape than other collagen varieties [31].
Because of these structural characteristics, Type IV collagen has a special ability it can form sheets. These sheets are a significant part of the structural makeup of the basement membrane in the skin.
This means that Type IV collagen has a distinct structure that allows it to create flexible, curved sheets, and you’ll find it playing a key role in the structure of the skin’s basement membrane [32, 33].
Type V
Type V collagen is like a manager collagen that helps regulate the formation of fibrils (which are like collagen threads).
It comes in at least three different versions – 1(V)2 2(V), 1(V)3, and 1(V)2(V)3(V). These versions are made by combining three different alpha chains – 1(V), 2(V), and 3(V) [34].
Type V collagen is not the main character in the extracellular matrix story; it’s more like a supporting actor. It links with other collagens like type I collagen, forming these mixed fibrils or thin threads with distinct characteristics [35].
Cells in various parts of our body make type V collagen, and its production is influenced by things like TGF- (transforming growth factor beta) and other growth factors [36].
Even though it can withstand digestion by certain enzymes [37], it’s not invincible – metalloproteinases and gelatinases (certain enzymes in the body) can break it down, helping in the remodeling (building) of the extracellular matrix [38].
Type V collagen is like a team player. It interacts with other collagen types and structural proteins, strengthening the scaffolding in our tissues.
It also interacts with matrix macromolecules, influencing how cells behave and function in our body [37]. Type V collagen plays a crucial role in maintaining the structure and function of our tissues.
Type VI
Collagen VI plays various roles in the tissues where it’s found, carrying out mechanical functions, protecting cells by inhibiting apoptosis (programmed cell death), and shielding against oxidative damage.
It also contributes to tumor development and progression by influencing cell differentiation and autophagic mechanisms [39].
This collagen type plays a role in anchoring cells and tissues, contributing to the overall stability of the extracellular matrix.
Type VII
Type VII collagen got its name because, at first, people thought it was an extra-long molecule, so they called it long-chain collagen.
This collagen is important in forming anchoring fibrils, which are like support beams providing stability to how the outer skin layer (epidermis) sticks to the deeper layer (dermis) at a specific interface called lamina lucida/papillary dermis [40].
Type VIII
Type VIII collagen is produced by several types of cells, including endothelial cells (those lining blood vessels), keratinocytes (cells in the outer layer of skin), mast cells (a type of immune cell), microvascular endothelial cells (tiny blood vessels), and even some tumor cells.
You can find it in different extracellular matrices, like in the white part of your eye (sclera), skin, and the tiny filters in your kidneys (glomerulus) [6, 41].
When it comes to its structure, Type VIII collagen is made up of two alpha chains, specifically, [alpha 1(VIII)2 alpha 2(VIII)] [42].
Its role in the body is still unknown, although recent studies suggest it’s relatively important in blood vessels.
Some research indicates that it may play a role in the movement of smooth muscle cells, which is critical for maintaining the structure of blood vessels.
Researchers speculate that Type VIII collagen might act as a kind of foundation for various cells, helping endothelial cells move around during the formation of new blood vessels (angiogenesis), aiding smooth muscle cells in penetrating the inner layer of blood vessels (intimal invasion) and assisting myofibroblasts during tissue scarring (fibrotic conditions) [43].
Type X
Type X collagen is a special member of the short-chain collagen family, mainly found in cartilage and crucial for bone growth and development.
It is primarily found in the growth plates of bones, where new bone formation occurs during development and growth.
The primary function of Type X collagen is to contribute to bone development and mineralization, particularly in the growth plates.
It’s like a marker for a specific type of mature cartilage cell called hypertrophic chondrocytes [44]. In humans, up to 18% of collagen synthesis in certain regions may be Type X.
Its role is believed to help in the process of calcification, potentially influencing the organization of the cartilage matrix.
Researchers believe Type X collagen is vital for understanding chondrocyte growth and differentiation. Mutations in this collagen type might be linked to certain bone development disorders [45].
Overall, Type X collagen provides perspective in cartilage biology, helping researchers learn more about bone growth and development.
Type XI
Type XI collagen plays a role in the body’s structural framework.
Acting as a fibrillary collagen, it’s widespread in various tissues like articular cartilage, testis, tendons, bone, muscles, placenta, lungs, and even the neoepithelium of the brain.
Its job is to regulate fibrillogenesis, which helps form collagen fibrils those thread-like structures holding our tissues together [46].
One of its functions is maintaining the spacing and diameter of type II collagen fibrils, acting like a supervisor for their proper formation. It also plays a role in kickstarting the formation of collagen types I and II [46].
It can bind with substances like heparin, heparan sulfate, and dermatan sulfate. However, despite its potential importance, we currently lack specific biomarkers to measure Type XI collagen [47].
Types XII, XIV, and XVI
Type XII collagen is like the supervisor in certain parts of our body – mainly found in the perichondrium (a layer around cartilage) and on the articular surface.
It’s a “homotrimeric” molecule, meaning it comprises three identical parts. Picture it as a big cross-shaped structure with specific domains that reach the space around collagen fibrils.
This collagen has two forms: a smaller one found in skin and such and a larger one discovered in epidermal cells [48].
Now, let’s talk about type XIV collagen. It’s similar but with a smaller cross-shaped structure. Type XIV collagen is more evenly spread in various tissues, interacting with type I collagen in places like skin, tendons, and more. It doesn’t directly bind to type I collagen but rather to a substance called decorin [48].
Lastly, we have type XVI collagen, synthesized by fibroblasts and myoblasts. It’s part of the show in the territorial matrix of chondrocytes, those cells in cartilage.
Imagine it as this integrated player in thin collagen fibrils, hanging out with types II and XI collagen.
It’s like a behind-the-scenes crew in different parts of our body, making sure things are structured just right [48].
Do You Need All Types Of Collagen?

To build collagen in the body, you need to have the building blocks of collagen the amino acids include glycine, proline, lysine, hydroxylysine, and hydroxyproline [49].
In addition, you need vitamin C to help form collagen in the body. Vitamin C is important for connective tissues because it allows an enzyme called prolyl 4-hydroxylase to do its job.
This enzyme is needed to change proline, a building block of proteins, and helps make and release procollagen.
You do not need to take in all the types of collagen as long as you get in enough of the building blocks i.e., amino acids that collagen is made of.
Collagen supplements, and even gelatine, all get broken down into glycine, proline, lysine, hydroxylysine, and hydroxyproline and can be used to build the various types of collagen in the body.
Does Collagen Source Matter?
Animal-derived collagen protein may not be suitable for vegetarian or vegan athletes.
While there are vegan and vegetarian products designed to replicate animal-based collagen if peptides unique to animal proteins are proven to possess distinct biological activity, vegetarian and vegan alternatives might be considered less efficient.
Further research is needed to assess the amino acid availability and effectiveness of vegan collagen substitutes.
Various animal-based collagen sources exhibit slight variations in their amino acid content, yet the differences are not significant enough to declare one type superior to another.
Table 1: Amino acid composition of the 5 major mammalian collagens and gelatin [50]
| Amino acid | Animal gelatin | |||||||
| Ox hide | Commercial bone | Pig skin | Ox-bone | Shark-skin | Lung-fish skin | Bone | Tendon | |
| Glycine | 27.5 | 27.2 | 26.4 | 25.3 | 26.5 | 24 | 25.8 | 25.4 |
| Leucine | 3.3 | 3.5 | 3.3 | 3.9 | 3.5 | 2.8 | 3.6 | 3.6 |
| Proline | 16.4 | 15.5 | 16.2 | 14.7 | 13.9 | 15.8 | 15.3 | 15.2 |
| Hydroxyproline | 14.1 | 13.3 | 13.5 | 14.1 | 10.9 | 10.8 | 14.1 | 12.6 |
| Hydroxylysine | 1.0 | 0.7 | 1.0 | 1.1 | 0.8 | 1.1 | 0.6 | |
Best Type Of Collagen
The debate on the superiority of collagen types remains unsettled due to their similar amino acid profiles. Type I collagen emerges as a strategic choice given its crucial role in reinforcing bones, muscles, and connective tissues.
The focus should be on a broad amino acid intake for overall collagen support. But for targeted benefits, leaning towards type I collagen might be your best bet.
References
- Abreu-Velez, A. M., & Howard, M. S. (2012). Collagen IV in Normal Skin and in Pathological Processes. N Am J Med Sci, 4(1), 1-8. doi:10.4103/1947-2714.92892
- Adam, M. P., Feldman, J., Mirzaa, G. M., Pagon, R. A., Wallace, S. E., Bean, L. J., . . . Amemiya, A. (1993). GeneReviews[Internet].
- Alcaide-Ruggiero, L., Molina-Hernndez, V., Granados, M. M., & Domnguez, J. M. (2021). Main and Minor Types of Collagens in the Articular Cartilage: The Role of Collagens in Repair Tissue Evaluation in Chondral Defects. Int J Mol Sci, 22(24). doi:10.3390/ijms222413329
- Aycock, R. S., & Seyer, J. M. (1989). Collagens of normal and cirrhotic human liver. Connective tissue research, 23(1), 19-31.
- Baar, K. (2017). Minimizing Injury and Maximizing Return to Play: Lessons from Engineered Ligaments. Sports Med, 47(Suppl 1), 5-11. doi:10.1007/s40279-017-0719-x
- Bakilan, F., Armagan, O., Ozgen, M., Tascioglu, F., Bolluk, O., & Alatas, O. (2016). Effects of Native Type II Collagen Treatment on Knee Osteoarthritis: A Randomized Controlled Trial. Eurasian J Med, 48(2), 95-101. doi:10.5152/eurasianjmed.2015.15030
- Birk, D. E. (2001). Type V collagen: heterotypic type I/V collagen interactions in the regulation of fibril assembly. Micron, 32(3), 223-237.
- Byers, P. H., Belmont, J., Black, J., De Backer, J., Frank, M., Jeunemaitre, X., . . . Sanders, L. (2017). Diagnosis, natural history, and management in vascular EhlersDanlos syndrome. Paper presented at the American Journal of Medical Genetics Part C: Seminars in Medical Genetics.
- Cao, Q., Mak, K. M., & Lieber, C. S. (2002). DLPC decreases TGF-1-induced collagen mRNA by inhibiting p38 MAPK in hepatic stellate cells. American Journal of Physiology-Gastrointestinal and Liver Physiology, 283(5), G1051-G1061.
- Chung, H. J., & Uitto, J. (2010). Type VII collagen: the anchoring fibril protein at fault in dystrophic epidermolysis bullosa. Dermatol Clin, 28(1), 93-105. doi:10.1016/j.det.2009.10.011
- Clifford, T., Ventress, M., Allerton, D. M., Stansfield, S., Tang, J. C. Y., Fraser, W. D., . . . Stevenson, E. (2019). The effects of collagen peptides on muscle damage, inflammation, and bone turnover following exercise: a randomized, controlled trial. Amino Acids, 51(4), 691-704. doi:10.1007/s00726-019-02706-5
- Di Martino, A., Cescon, M., D’Agostino, C., Schilardi, F., Sabatelli, P., Merlini, L., & Faldini, C. (2023). Collagen VI in the Musculoskeletal System. Int J Mol Sci, 24(6). doi:10.3390/ijms24065095
- Dong, C., & Lv, Y. (2016). Application of Collagen Scaffold in Tissue Engineering: Recent Advances and New Perspectives. Polymers (Basel), 8(2). doi:10.3390/polym8020042
- Ellingson, A. J., Pancheri, N. M., & Schiele, N. R. (2022). Regulators of collagen crosslinking in developing and adult tendons. Eur Cell Mater, 43, 130-152. doi:10.22203/eCM.v043a11
- Frantz, C., Stewart, K. M., & Weaver, V. M. (2010). The extracellular matrix at a glance. J Cell Sci, 123(Pt 24), 4195-4200. doi:10.1242/jcs.023820
- Hasegawa, H., Naito, I., Nakano, K., Momota, R., Nishida, K., Taguchi, T., . . . Ohtsuka, A. (2007). The distributions of type IV collagen chains in basement membranes of human epidermis and skin appendages. Archives of histology and cytology, 70(4), 255-265.
- Holwerda, A. M., & van Loon, L. J. C. (2022). The impact of collagen protein ingestion on musculoskeletal connective tissue remodeling: a narrative review. Nutr Rev, 80(6), 1497-1514. doi:10.1093/nutrit/nuab083
- Horn, D., Siebert, E., Seidel, U., Rost, I., Mayer, K., Abou Jamra, R., . . . Kornak, U. (2017). Biallelic COL3A1 mutations result in a clinical spectrum of specific structural brain anomalies and connective tissue abnormalities. American journal of medical genetics Part A, 173(9), 2534-2538.
- Jrgensen, A., Fagerheim, T., Rand-Hendriksen, S., Lunde, P. I., Vorren, T. O., Pepin, M. G., . . . Byers, P. H. (2015). Vascular EhlersDanlos syndrome in siblings with biallelic COL3A1 sequence variants and marked clinical variability in the extended family. European Journal of Human Genetics, 23(6), 796-802.
- Kannus, P. (2000). Structure of the tendon connective tissue. Scand J Med Sci Sports, 10(6), 312-320. doi:10.1034/j.1600-0838.2000.010006312.x
- Kapandji, I. (1977). The physiology of the joints. Churchill Livingstone, 2, 186-189.
- Khoshnoodi, J., Pedchenko, V., & Hudson, B. G. (2008). Mammalian collagen IV. Microsc Res Tech, 71(5), 357-370. doi:10.1002/jemt.20564
- Konomi, H., Hayashi, T., Nakayasu, K., & Arima, M. (1984). Localization of type V collagen and type IV collagen in human cornea, lung, and skin. Immunohistochemical evidence by anti-collagen antibodies characterized by immunoelectroblotting. The American journal of pathology, 116(3), 417.
- Kuivaniemi, H., & Tromp, G. (2019). Type III collagen (COL3A1): Gene and protein structure, tissue distribution, and associated diseases. Gene, 707, 151-171. doi:10.1016/j.gene.2019.05.003
- Lian, C., Wang, X., Qiu, X., Wu, Z., Gao, B., Liu, L., . . . Peng, Y. (2019). Collagen type II suppresses articular chondrocyte hypertrophy and osteoarthritis progression by promoting integrin 1 SMAD1 interaction. Bone research, 7(1), 8.
- Luo, Y. Y., & Karsdal, M. A. (2016). Chapter 11 – Type XI Collagen. In M. A. Karsdal (Ed.), Biochemistry of Collagens, Laminins and Elastin (pp. 77-80): Academic Press.
- Mak, K. M., Png, C. Y., & Lee, D. J. (2016). Type V Collagen in Health, Disease, and Fibrosis. Anat Rec (Hoboken), 299(5), 613-629. doi:10.1002/ar.23330
- Malfait, F., Francomano, C., Byers, P., Belmont, J., Berglund, B., Black, J., . . . Burrows, N. P. (2017). The 2017 international classification of the EhlersDanlos syndromes. Paper presented at the American Journal of Medical Genetics Part C: Seminars in Medical Genetics.
- Miller, E. J., Epstein Jr, E. H., & Piez, K. A. (1971). Identification of three genetically distinct collagens by cyanogen bromide cleavage of insoluble human skin and cartilage collagen. Biochemical and Biophysical Research Communications, 42(6), 1024-1029.
- Moriya, K., Bae, E., Honda, K., Sakai, K., Sakaguchi, T., Tsujimoto, I., . . . Sakai, T. (2011). A fibronectin-independent mechanism of collagen fibrillogenesis in adult liver remodeling. Gastroenterology, 140(5), 1653-1663.
- Muragaki, Y., Jacenko, O., Apte, S., Mattei, M., Ninomiya, Y., & Olsen, B. R. (1991). The alpha 2 (VIII) collagen gene. A novel member of the short chain collagen family located on the human chromosome 1. Journal of Biological Chemistry, 266(12), 7721-7727.
- Myllyharju, J., & Kivirikko, K. I. (2004). Collagens, modifying enzymes and their mutations in humans, flies and worms. TRENDS in Genetics, 20(1), 33-43.
- Nah, H. D., Swoboda, B., Birk, D. E., & Kirsch, T. (2001). Type IIA procollagen: expression in developing chicken limb cartilage and human osteoarthritic articular cartilage. Developmental Dynamics: An Official Publication of the American Association of Anatomists, 220(4), 307-322.
- Naomi, R., Ridzuan, P. M., & Bahari, H. (2021). Current Insights into Collagen Type I. Polymers (Basel), 13(16). doi:10.3390/polym13162642
- Olsen, B. R. (1995). New insights into the function of collagens from genetic analysis. Current opinion in cell biology, 7(5), 720-727.
- Patel, K., Munir, D., & Santos, R. (2022). Beneficial use of animal hides for abattoir and tannery waste management: a review of unconventional, innovative, and sustainable approaches. Environmental Science and Pollution Research, 29. doi:10.1007/s11356-021-17101-5
- Plancke, A., Holder-Espinasse, M., Rigau, V., Manouvrier, S., Claustres, M., & Van Kien, P. K. (2009). Homozygosity for a null allele of COL3A1 results in recessive EhlersDanlos syndrome. European Journal of Human Genetics, 17(11), 1411-1416.
- Plenz, G. A., Deng, M. C., Robenek, H., & Vlker, W. (2003). Vascular collagens: spotlight on the role of type VIII collagen in atherogenesis. Atherosclerosis, 166(1), 1-11.
- Ricard-Blum, S. (2011). The collagen family. Cold Spring Harb Perspect Biol, 3(1), a004978. doi:10.1101/cshperspect.a004978
- Schmid, T. M., & Linsenmayer, T. F. (1990). Immunoelectron microscopy of type X collagen: supramolecular forms within embryonic chick cartilage. Dev Biol, 138(1), 53-62. doi:10.1016/0012-1606(90)90176-j
- Shen, G. (2005). The role of type X collagen in facilitating and regulating endochondral ossification of articular cartilage. Orthod Craniofac Res, 8(1), 11-17. doi:10.1111/j.1601-6343.2004.00308.x
- Shuttleworth, C. A. (1997). Type VIII collagen. Int J Biochem Cell Biol, 29(10), 1145-1148. doi:10.1016/s1357-2725(97)00033-2
- Smith, S. M., & Melrose, J. (2019). Type XI collagenperlecanHS interactions stabilise the pericellular matrix of annulus fibrosus cells and chondrocytes providing matrix stabilisation and homeostasis. Journal of Molecular Histology, 50(3), 285-294. doi:10.1007/s10735-019-09823-1
- Sderhll, C., Marenholz, I., Kerscher, T., Rschendorf, F., Esparza-Gordillo, J., Worm, M., . . . Rohde, K. (2007). Variants in a novel epidermal collagen gene (COL29A1) are associated with atopic dermatitis. PLoS biology, 5(9), e242.
- Sorushanova, A., Delgado, L. M., Wu, Z., Shologu, N., Kshirsagar, A., Raghunath, R., . . . Zeugolis, D. I. (2019). The Collagen Suprafamily: From Biosynthesis to Advanced Biomaterial Development. Adv Mater, 31(1), e1801651. doi:10.1002/adma.201801651
- Uzawa, K., Kasamatsu, A., & Yamauchi, M. (2023). Collagen crosslinking in oral cancer. Oral Science International, 21. doi:10.1002/osi2.1182
- van der Rest, M., & Garrone, R. (1991). Collagen family of proteins. Faseb j, 5(13), 2814-2823.
- Von Der Mark, K. (2006). CHAPTER 1 – Structure, Biosynthesis and Gene Regulation of Collagens in Cartilage and Bone. In M. J. Seibel, S. P. Robins, & J. P. Bilezikian (Eds.), Dynamics of Bone and Cartilage Metabolism (Second Edition) (pp. 3-40). Burlington: Academic Press.
- Wolff, K., Goldsmith, L. A., Katz, S. I., Gilchrest, B. A., Paller, A. S., & Leffell, D. J. (2008). Fitzpatrick’s dermatology in general medicine: McGraw-Hill New York.
- YANG, C. L., RUI, H., MOSLER, S., NOTBOHM, H., SAWARYN, A., & MLLER, P. K. (1993). Collagen II from articular cartilage and annulus fibrosus: Structural land functional implication of tissue specific posttranslational modifications of collagen molecules. European journal of biochemistry, 213(3), 1297-1302.




